Information at the level of health systems will be important for better policy making and charting out reform agenda for change. The reform agenda for mental hospitals of Kerala has not, as yet taken off, though it has long been repeatedly articulated since 1979 (Pai committee report). The latest of such reports being the 6th estimate committee report (PDF) (2012) by the legislature under V D Satheesan MLA. A lack of a mental health information system which can capture data on health system variables may have contributed to the reform gap.
I have collated here, data on a few variables which I felt was important. These data were requested from the three government mental hospitals (GMHCs –Government Mental Health Centres) through RTI (Right To Information Act, 1987) query to the public information officers of these institutions. The data on financing of the institutions was collected from the annual plan document 2013-14, Government Of Kerala, which is available in the public domain. Data points (see Table 1) are clustered under three domains and certain data points are elaborated and commented upon in the discussion.
Table 1 (Data on certain health system vartiables about GMHCs) 
(1) Admission and Discharge: Total admission in 2014 was 7113 out of which 874 (12%) were admitted via reception order under Mental Health Act. (Unfortunately I did not ask for the number of prisoner patients admitted, therefore this data is not available)
A total of 154 patients as on 2014 are admitted and staying the Mental Hospitals for more than 10 years out of which 100 are in GMHC, Kozhikode. In absence of a plan for this subset of patients it is possible that these patients will remain in the centers for the rest of their lives. It was reported that a total of 60 patients were discharged and transferred to private rehabilitation homes.
A possible alternative could be to contact the Dept. of housing of Gov. of Kerala and explore means for building permanent housing for them. Any of the GMHCs could pilot a model of supported housing for these patients.
(2) Staff pattern sanctioned and currently present: Till date, shortage of staff in GMHCs had been a persistent problem. Thanks to proactive measures by the government via post creation (See here ) shortage is being steadily rectified. Currently sanctioned posts for doctors are steadily getting filled though the requirement as put by the centers are very high (Click to see a table from appendix of CAG performance aduit report).
We can see that currently, there is no shortage for doctors in sanctioned posts but shortage of other professionals does exist.
(3) Financing available to the institutions in the year 2014-15 is 323903 thousand rupees (32.39 crores) of which 28 crores( 86.44%) goes towards salary of personnel. During the corresponding period money allotted to community mental health services of all 14 districts was 4.79 crores.
Much of the annual state budgetary allocation for mental health under the health budget currently goes to the three mental hospitals of Kerala.
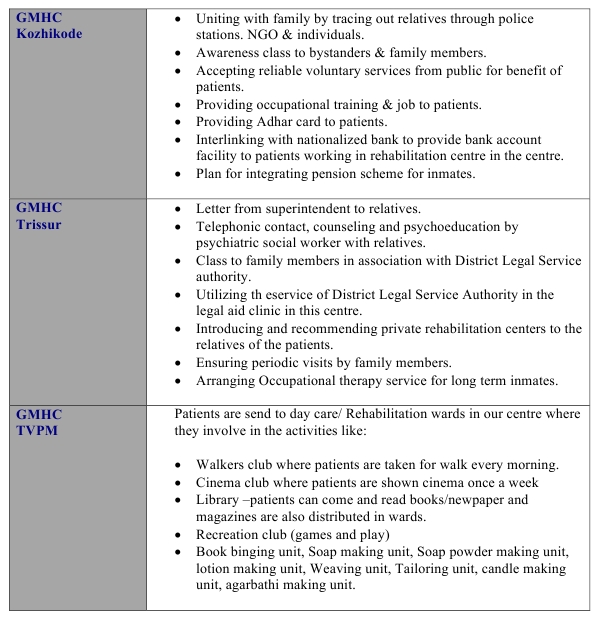
Tail piece: Regarding the reply to the question on “how many patients are currently admitted and staying more than two years” : as the question was little ambiguous the figures may not be reliable, nevertheless the total number is 273. These patients were engaged in various activities in the centers as per table 2. I am afraid many of these interventions may not pass the test of a rigorous state of the art evidence-based-rehabilitation techniques of modern times.
Table 2 (Activities in GMHCs for patients staying more than 2 years)
PS: A quick look at the impact of DMHP on IP and OP of Mental hospitals is pertinent (document extracts)
- The programme has been so successful in the district that it brought down the number of OP and in- patients at the mental health Centre by more than half, and even received a commendation from the WHO. DMHP Tvpm currently has about 2000 regular patients across the district. Dmhp annual activity report 2011-12 (PDF)
- The implementation of the DMHP/CMHP in four districts (Kasargode, Kozhikode, Malappuram and Wayanad) by IMHANS helped to reduce the workload of MHC, Kozhikode as evidenced by the reduction (22.61 per cent) in intake of inpatients at MHC, Kozhikode from 31,802 (2005) to 24,610 (2009). According to the cost-effect analysis of the MHC, Kozhikode made by the Institute during the year 2009, there was saving of 26.15 per cent in expenditure on diet, medicine and drugs due to reduction in intake of inpatients. Bed strength and average occupancy per day during 2005-10 in MHCs (Kozhikode, Thiruvananthapuram, and Thrissur) revealed that the percentage of occupancy ranged between 102 and 118. The excess occupancy was due to overstay of improved patients, heavy admission of relapsed cases, non- utilisation of new wards due to shortage of staff and non-completion of works, etc. Overstay of patients was due to non-availability of adequate rehabilitation centres, non-availability of proper address of the patients who were admitted by court orders, non-acceptance of recovered patients by their families etc. The three MCHs had a total bed strength of 154 (Kozhikode: 71, Thiruvananthapuram: 43 and Thrissur: 40).(?? Tvpm has 570 beds, KKD 474 as per another report) The average bed occupancy per day during 2005-10 was 42, 40 and 18 in MCHs, Thiruvananthapuram, Kozhikode and Thrissur respectively. CAG performance audit 2010 (PDF)
- The mental health centre was an ally of the primary care programme and benefited from the newly- integrated services through for example, fewer referrals. WHO-WONCHA report 2008 (PDF)
(Added on Aug,10, 2015) The data from this post got represented in an infographic (see below) which came in Times of India article.
29.03.2021….came across this old article in IJP (PDF) and the figures from it which is posted below (long stay defined as 2yrs and above)




added on 30.06.2021: Hans Foundation report in 2019 show number of patients staying more than one year

latest figures on long stay from kerala: added on august5 , 2021

At the Government Mental Health Centre in Peroorkada, 162 persons have recovered and are awaiting rehabilitation. Of them, 103 are men and 59, women. Their relatives have not come forward to take them home.
At the Mental Health Centre in Thrissur, 69 persons are waiting for rehabilitation, of which 28 are women and 41, men. At the Kozhikode Mental Health Centre, 80 persons have to be rehabilitated, out of whom 25 have been shifted to various rehabilitation centres this year.
Mental health hospitals to get rehabilitation centres: TheHindu aug 4, 2021

video of same in youtube https://www.youtube.com/watch?v=bRamut2KaZg
added on 21.08.2021: developments based on suomotoc ase taken by kerala high court towards rehab of prisoners languishing in state mental hospitals
https://www.deshabhimani.com/news/kerala/high-court-jail-mental-health-centre/963766
(പ്രശാന്ത് നായർ ഐഎഎസ് എഴുതി ഡിസി ബുക്സ് പ്രസിദ്ധീകരിച്ച ‘കളക്ടർ ബ്രോ ഇനി ഞാൻ തള്ളട്ടെ’, എന്ന പുസ്തകത്തിലെ പേജ് നമ്പർ 69മുതൽ 74വരെയുള്ള പ്രസക്ത ഭാഗങ്ങൾ )
………..സബ് ജഡ്ജ് ശ്രീ.ആർ.എൽ.ബൈജുവിനൊപ്പം കുതിരവട്ടത്തെ സർക്കാർ മാനസികാരോഗ്യ കേന്ദ്രം സന്ദർശിക്കുമ്പോൾ നിയമപരമായി ഒരു കടമ നിർവഹിക്കുന്നു എന്നതിനപ്പുറം മറ്റൊന്നും മനസ്സിലുണ്ടായിരുന്നില്ല. എന്നാൽ ആ ദിവസം, പിന്നീട് വരാനിരിക്കുന്ന എന്റെ എല്ലാ ദിവസങ്ങളെയും മാറ്റിമറിച്ചു.
മാനസികാരോഗ്യ കേന്ദ്രത്തിലെ ജനറൽ വാർഡുകൾ കുട്ടിക്കാലത്ത് ഞങ്ങൾ തിരുവനന്തപുരം മൃഗശാലയിൽ കണ്ട ഇരുമ്പു കൂടുകളെ ഓർമ്മിപ്പിച്ചു.പുരുഷന്മാരുടെ വാർഡിൽ ഒരിടുങ്ങിയ മുറിയിൽ 30-40 രോഗികൾ തിങ്ങിക്കൂടി കഴിയുന്നത് കണ്ടു.ഓരോരുത്തരും അവനവന്റെ കുഞ്ഞു വലിയ ലോകത്തായിരുന്നെന്ന് മാത്രം.ഒരു അന്തേവാസി യോട് ഇരുമ്പഴികൾക്കുള്ളിലൂടെ ഞാൻ സംസാരിച്ചു.രണ്ടുദിവസം മുമ്പ് ദുബായിൽ നിന്ന് തിരിച്ചെത്തിയ ഒരു പ്രവാസി വ്യവസായിയാണ് താനെന്ന് അയാൾ സ്വയം പരിചയപ്പെടുത്തി. വിമാനത്താവളത്തിൽ എത്തിയ ഉടനെ അദ്ദേഹത്തിന് ചില മാനസിക ബുദ്ധിമുട്ടുകൾ അനുഭവപ്പെടുകയും ബന്ധുക്കൾ അദ്ദേഹത്തെ നേരെ കുതിരവട്ടം ആശുപത്രിയിലേക്ക് കൊണ്ടു വരികയും ചെയ്തു.എല്ലാം എത്ര പെട്ടെന്നാണ്! നമ്മുടെ മാനസികനില എത്രവേഗം മാറി മറിയാമെന്ന തിരിച്ചറിവ് എന്നെ ഭയപ്പെടുത്തി. നമ്മൾ ഒരു പുതിയ താമസസ്ഥലത്തേക്ക് മാറുമ്പോൾ ചുറ്റുവട്ടത്ത് നല്ല സ്കൂളുകളും ആശുപത്രികളും ഉണ്ടോ എന്ന് അന്വേഷിക്കാറുണ്ടല്ലോ.എന്നാൽ അവിടെ കൊള്ളാവുന്ന ഒരു മാനസിക ആരോഗ്യ കേന്ദ്രം ഉണ്ടോ എന്ന് നമ്മളാരും തിരക്കാറില്ല. എന്തുവന്നാലും നമ്മുടെ മനോനില സുസ്ഥിരമായി തുടരുമെന്ന് നമ്മൾ അങ്ങ് വെറുതെ വിശ്വസിക്കുകയാണ്.എന്നാൽ ആ അന്തേവാസിയുടെ കഥ എന്നെ ഞെട്ടിച്ചുകളഞ്ഞു. മനുഷ്യന്റെ മാനസികാരോഗ്യം ശരിക്കും ഞാണിന്മേൽ കളിയാണ്.ആശുപത്രി സൂപ്രണ്ടിനോട് ഞാനാ രോഗിയുടെ കാര്യം വിശദമായി ചോദിച്ചു.അദ്ദേഹത്തിന്റെ മറുപടി ഇങ്ങനെയായിരുന്നു,’അയാൾ പറഞ്ഞതെല്ലാം ശരിയാണ്.പക്ഷേ ചെറിയൊരു തിരുത്തുണ്ട്.അയാൾ നാട്ടിലേക്ക് തിരിച്ചു വന്നതും ഇവിടെ അഡ്മിറ്റ് ആയതും 15 കൊല്ലം മുമ്പാണെന്നു മാത്രം’.
രോഗം ഭേദമായിട്ടും മടങ്ങിപ്പോകാനൊരിടമില്ലാത്ത ധാരാളം പേരുണ്ടായിരുന്നു അവിടെ. പലരെയും വീട്ടുകാർ ഉപേക്ഷിച്ചിരുന്നു. അക്രമാസക്തരായ രോഗികളെ പാർപ്പിച്ചിരുന്ന ഒറ്റപ്പെട്ട മുറികളിലേക്കാണ് ഞാൻ പിന്നീട് പോയത്.സദാസമയം പൂട്ടിയിടുന്ന അഴികളുള്ള സോളിട്ടറി സെല്ലുകൾ.അവിടെ കണ്ട കാഴ്ച ഞാനൊരിക്കലും മറക്കില്ല.സ്വന്തം മലവും ഭക്ഷണാവശിഷ്ടങ്ങളും പുരണ്ട നഗ്നശരീരവുമായി ഓരോ രോഗിയും അവനവന്റെ ചെറിയ മുറിക്കുള്ളിൽ കിടക്കുന്നു.ചിലരെല്ലാം സെഡേഷനിലാണ്.സെല്ലിന്റെ ഒരു മൂലയ്ക്ക് കിടക്കാനുള്ള സൗകര്യമുണ്ട്.അകത്തോട്ട് സ്റ്റീലിൽ തീർത്ത കക്കൂസ്.സിറാമിക് ക്ലോസെറ്റുകൾ അവർ തല്ലിപ്പൊട്ടിക്കുകയും മൂർച്ചയുള്ള കഷണങ്ങൾ എടുത്ത് സ്വയം പരിക്കേൽപ്പിക്കുകയും ചെയ്യുമത്രേ.ഉടുതുണി കീറിക്കളയാനും ആത്മഹത്യയ്ക്ക് ഉപയോഗിക്കാനും പ്രവണതയുള്ളവരാണിവരിൽ പലരും.ഒരു മുറിയിലെ മങ്ങിയ വെട്ടത്ത് കണ്ടത്,ഷീസോഫ്രീനിയയുടെ അങ്ങേയറ്റമെത്തിയ ഒരു രോഗിയെ.മറ്റൊരു അന്തേവാസിയെ കൊലപ്പെടുത്തിയ ചരിത്രമുള്ളയാൾ.ഒടുവിലത്തെ മുറിയിലെ കാഴ്ച കണ്ട് എന്റെ കാൽമുട്ടുകളുടെ ബലം ചോർന്നുപോയി. മുറിക്കുള്ളിൽ നട്ടെല്ലും തോളെല്ലുകളുമുന്തിയ പ്രായം ചെന്ന ഒരു മനുഷ്യൻ. ശ്രദ്ധയോടെയും ക്ഷമയോടെയും അയാൾ അകത്തെ മൂലയ്ക്കുള്ള സ്റ്റീൽ കക്കൂസിൽ കൈയ്യിട്ട് സ്വന്തം മലം തോണ്ടിയെടുത്ത് ഭക്ഷിക്കുന്നു.താടിരോമങ്ങളിൽ മലവും തുപ്പലുമൊലിച്ചിറങ്ങുന്നുണ്ടായിരുന്നു.തന്റെ നഗ്ന ദേഹം ഞങ്ങൾക്ക് നേരെ തിരിച്ചു കൊണ്ട് അയാൾ സായിപ്പിന്റെ ഇംഗ്ലീഷിൽ എന്തോ പറഞ്ഞു.എന്റെ കണ്ണുകൾ നീറി.എന്റെ വയർ ആരോ ചുരുട്ടിക്കൂട്ടിയതുപോലെ.സഹനശേഷിയുടെ എല്ലാ അതിർ വരമ്പും കടന്നു കഴിഞ്ഞിരുന്നു.സെല്ലുകളുടെ ഭാഗത്തുനിന്നും ഞാൻ വേഗം പുറത്തേക്കോടി.
നോർമലായെന്ന് സ്വയം വിശ്വസിപ്പിച്ച് ആശുപത്രി സൂപ്രണ്ടിനോട് അവിടെ അടിയന്തരമായി വേണ്ട സൗകര്യങ്ങൾ എന്തെല്ലാമാണെന്ന് ഞാൻ ചോദിച്ചു. അടിയന്തരമായി രണ്ടരക്കോടിയോളം രൂപ വെള്ളത്തിന്റെയും കറണ്ടിന്റെയും കുടിശ്ശിക ബില്ലടയ്ക്കാനുണ്ട്. ദൈനംദിന ചെലവുകൾ കൂടിക്കൂടി വരുമ്പോഴും ബജറ്റിലെ നീക്കിയിരിപ്പ് തുക എല്ലാ വർഷവും കുറഞ്ഞുവരികയാണ്. തിരുവനന്തപുരത്തിരുന്ന് ബജറ്റ് തയ്യാറാക്കുന്ന ഉദ്യോഗസ്ഥർക്കെന്ത് കുതിരവട്ടവും സംക്രാന്തിയും!…………………………………………………………….. മാനസികരോഗ ആശുപത്രിയോ അവിടുത്തെ അന്തേവാസികളോ അധികാരികളുടെ മുൻഗണനാ പട്ടികയിലില്ലായിരുന്നു.അവർക്ക് വേണ്ടി ശബ്ദമുയർത്താൻ നേതാക്കളോ യൂണിയനുകളോ ബന്ധുക്കളോ ഉണ്ടായിരുന്നില്ല.ഏറ്റവും പ്രധാനപ്പെട്ട കാര്യം അവർക്ക് വോട്ടവകാശമില്ല എന്നതാണ്. ജനാധിപത്യ സംവിധാനം ഭ്രഷ്ട് കൽപ്പിച്ച മനുഷ്യരാണവർ…………………………………………………………. ഏതൊരു മാനസികാരോഗ്യ കേന്ദ്രത്തിലെയും അടിസ്ഥാന ഉപകരണങ്ങളിലൊന്നാണ് ഇലക്ട്രോ കോൺവൾസീവ് തെറാപ്പി മെഷീൻ.സിനിമയിൽ കണ്ടു കാണും,ഷോക്കടിപ്പിക്കുന്ന യന്ത്രം. 15 വർഷമായി ആ ആശുപത്രിയിൽ അങ്ങനെയൊന്ന് ഇല്ലായിരുന്നുവെന്നു പറഞ്ഞാൽ വിശ്വസിക്കാൻ പ്രയാസമായിരിക്കും.ഏതായാലും സ്പോൺസർഷിപ് വഴി ഞങ്ങൾ ഒരു യന്ത്രം ഒപ്പിച്ചു. 2015 ജൂലൈയിൽ മെഷീൻ ലഭിച്ചശേഷം ആശുപത്രി സൂപ്രണ്ട് ഏതാണ്ട് 30 മാസത്തോളം ഓഫീസുകൾ പലതു കയറിയിറങ്ങിയ ശേഷമാണ് അത് സുരക്ഷിതമായി പ്രവർത്തിക്കാനാവശ്യമായ ഒരു അനസ്തേറ്റിസ്റ്റിന്റെ സേവനം ലഭ്യമായത്. ഉദ്യോഗസ്ഥപ്രഭുത്വമെന്ന ഭീകരസത്വം നമ്മളെ ഭയപ്പെടുത്തും.കോഴിക്കോട്ടുനിന്ന് ഞാൻ സ്ഥലം മാറിപ്പോയി പിന്നെയും മാസങ്ങൾക്കുശേഷം 2017 നവംബർ 28നാണ് ഈ യന്ത്രം പ്രവർത്തനക്ഷമമായത്.ജില്ലാ മെഡിക്കൽ ഓഫീസർ ഡോ.സരിത ഇത് ശരിയാക്കാൻ വലിയ പങ്കാണ് വഹിച്ചത്.ഇന്ന് സംസ്ഥാന ആരോഗ്യവകുപ്പ് ഡയറക്ടറാണ് അവർ.
ഒന്ന് ചിന്തിച്ചാൽ സമയം ഒരു അത്ഭുത പ്രതിഭാസമാണ്. മനസ്സിന്റെ സമനിലതെറ്റിയ ഒരാൾ താൻ ആശുപത്രിയിൽ എത്തിയിട്ട് രണ്ടു ദിവസമേ ആയുള്ളൂ എന്ന് വിചാരിച്ചു വർഷങ്ങൾ കഴിച്ചുകൂട്ടുന്നു.മറുവശത്ത് ഒരു ഡോക്ടർ രോഗികളെ ചികിത്സിക്കാനുള്ള യന്ത്രം പ്രവർത്തിക്കാനുള്ള ആളെ കണ്ടെത്താനായി ജീവിതത്തിന്റെ രണ്ടു വർഷത്തിലധികം ചെലവഴിക്കുന്നു.നമ്മളോ,സിനിമാ തീയേറ്ററിലെ ക്യൂവിൽ രണ്ടുമിനിറ്റ് വൈകിയാൽ ചുറ്റുമുള്ളതെന്തിനെയും പ്രാകുന്നു.എല്ലാം ഓരോരുത്തരുടെ സമയം.
ആശുപത്രിയിലേക്കുള്ള ആദ്യ സന്ദർശനങ്ങളിലൊന്നിലാണ് അവിടുത്തെ ഭക്ഷണക്രമം 1979-ൽ നിശ്ചയിച്ചതാണെന്ന് അറിഞ്ഞത്.അതിനോടകം,അവിടുത്തെ കാര്യങ്ങൾ കേട്ട് ഞെട്ടുന്നത് ഞാൻ നിർത്തിയിരുന്നു.ഗോതമ്പ് കഞ്ഞിയായിരുന്നു മെനുവിലെ പ്രധാന ഇനം.ഗോതമ്പ് കഞ്ഞി മാത്രം കൊടുത്തു വർഷങ്ങളോളം പൂട്ടിയിട്ടാൽ,പൂർണ്ണ മാനസികാരോഗ്യമുള്ള ഒരാൾക്ക് പോലും സമനില തെറ്റാം.1979 മുതൽ ആ ആഹാരരീതി പരിഷ്കരിക്കണമെന്ന് ഒരാൾക്ക് പോലും തോന്നിയില്ല എന്നതായിരുന്നു ആശ്ചര്യപ്പെടുത്തിയ കാര്യം.കേരളത്തിന് തീരെ അപരിചിതമായ ഗോതമ്പു കഞ്ഞി എന്തുകൊണ്ടും മെനുവിൽ ഉൾപ്പെടുത്തിയെന്നതുതന്നെ അജ്ഞാതമാണ്. ഒരുപക്ഷേ അക്കാലത്ത് അരിക്ക് ക്ഷാമമുണ്ടായിരുന്നിരിക്കാം.എന്താണെന്ന് എനിക്ക് ശരിക്കുമറിയില്ല.പക്ഷേ,ഒന്നുറപ്പാണ്.ഈ വലിയ ജനാധിപത്യ ലോകത്ത് എന്തോ ഒന്നിന് കടുത്ത ക്ഷാമമുണ്ടായിരുന്നു. തീർച്ച.

There’s a place in Thalikulam, Kerala, where low price houses are available. This trust is set up by Dr P Mohamed Ali, leading businessman of middle-east who belongs to kerala. Check out his website to know about this place : http://www.authorstream.com/Presentation/akruti182440-2505600-talikulam-vikas-trust-press-release/
LikeLike
Thanks for the info…
LikeLike